The need for professional services in obesity surgery is increasing. Also in Thun and the surrounding area. And so it was only a logical step that the clinic of Dr. Naef in Thun now became part of the network of specialized facilities of Swiss1Chirurgie. You can learn more about this in the article.
Continue readingWorld Obesity Day 2022 – All must act
“Everybody needs to act” – This is the motto of World Obesity Day on 04 March 2022. Find out how Swiss1Chirurgie sees the effort against the worldwide affliction of obesity and what is expected from all of us in the Swiss1Chirurgie statement.
Continue readingThe COVID19 virus and obesity – a dangerous combination
Since the beginning of 2020, and probably even before, the COVID-19 virus, which is considered dangerous, has been rampant throughout the world. The pandemic development summarised under the collective term Corona crisis has far-reaching consequences for all life in the world – also in Switzerland. Even if the infection figures and the number of deaths caused by COVID-19 are currently declining, the virus has not gone away. It is still there. And in many countries there is and growing fear that a second high wave of infection can be expected in autumn at the latest.
Evaluate risk groups correctly
In principle, it can be assumed that almost anyone can be infected by the Corona virus. Across age groups, social boundaries and income groups, the virus can affect anyone. Protective measures such as social distancing, wearing mouth and nose masks and maintaining good hand hygiene can significantly reduce the risk of infection, but not eliminate it.
With the statistical collection and evaluation of data on the course of the Corona pandemic and its spread, certain risk groups have been defined whose risk of infection is clearly and measurably above average. Currently known risk groups include
- in principle, all persons aged 65 and over
- People with high blood pressure
- Adults with chronic respiratory diseases
- Diabetics of both levels
- Men and women with diseases and therapies associated with a weakened immune system
- all people with cardiovascular diseases and
- Cancer patients.
Many of these diagnoses also apply to severely overweight people who have a BMI of over 40 and are thus classified as severely obese.
Obesity and corona form a dangerous combination
Interesting and at the same time worrying is the combination of obesity and an infection with the COVID-19 virus. After all, chronic obesity is often associated with risk factors such as high blood pressure, fatigue, diabetes, a weakened immune system, cardiovascular problems and a lifestyle that is accompanied by little exercise in the fresh air.
In this constellation, very overweight people are particularly often found in the risk groups for corona infection. This means that significantly obese adults in particular are at substantially greater risk of infection.
What we recommend to patients with obesity
In the dangerous connection between obesity and the risk of corona infection described above, we recommend that people who are significantly overweight receive accompanying advice and care from a specialist, for example from the obesity surgery doctors in the Swiss1Chirurgie and Centre for Bariatric Surgery (ZfbC) clinics. Here, people are aware of the entire problem of obesity, especially in connection with the COVID19 virus, and can give the decisive tips.
In addition, affected patients are advised to seek treatment at the Swiss1Chirurgie obesity centres before the expected arrival of the second wave of infection. In addition to thorough diagnosis and advice on individual treatment options for morbid obesity, the specialists at Swiss1Chirurgie and ZfbC offer comprehensive advice on preventive options for sufferers with regard to possible COVID-19 disease.
Focus on dietary and lifestyle changes
Given the particular vulnerability of overweight people with a BMI of 40 or more, it is strongly advised that they immediately change their entire diet and lifestyle to a healthier option. What is so easy to put into words here poses great challenges for most of those affected.
Therefore, specialist counselling and care is an option that should definitely be used, not only with regard to the risk from the COVID19 virus. This is because overweight people in particular often have an accumulation of risk factors that favour both infection with the corona virus and a comparatively more problematic course of the disease.
Irrespective of the current corona pandemic, we strongly advise overweight people to seek specialist advice, treatment and care, for example in the Swiss1Chirurgie obesity surgery clinics. Not only does this effectively counteract the risk of a severe course of COVID-19 infection, but it is also a promising first step towards a healthier future overall.
Grade III obesity as a risk factor for a more severe course of COVID-19
is officially on the list as of today: Annex 6 of COVID Regulation 2, adaptation of 14 May 2020, item 7.
Communication from: Eidgenössisches Departement des Innern EDI Bundesamt für Gesundheit BAG Direktionsbereich Öffentliche Gesundheit Sektion Prävention in der Gesundheitsversorgung
Medical expertise and expert advice on Radio Bern1
People are more interested in their health and use different sources to inform themselves about healthy lifestyles but also about diseases and their symptoms as well as treatment options. Especially widespread diseases such as obesity (morbid overweight) or reflux diseases (for example chronic acid reflux) are moving further into the focus of public interest and thus also opening the doors to media such as radio or television.
Swiss1 Surgery, led by Prof. Jörg Zehetner, has long been committed to professional public relations and welcomes all measures and ways to promote social awareness of such diseases. Jörg Zehetner sees the stigmatisation of affected women and men as a problem that prevents many patients from undergoing appropriate medical examinations. Ultimately, this leads to a vicious circle, which is associated with a long path of suffering and rarely leads to an improvement in the lives of those affected, usually not at all. Old but also new widespread diseases are not only a problem for those affected themselves. The economy and society as a whole are also affected when rising case numbers lead to more incapacity to work, occupational disability, disability to work and, ultimately, rising health insurance costs.
With a lot of commitment, Jörg Zehetner has therefore now spoken out on the radio as part of his efforts to be heard more in public. On 17 August 2020, as part of the podcast series “Medical Knowledge”, the topic of oesophagectomy (resection of the oesophagus) was a focal point on which the specialist physician at the Hirslanden Klinik Beau Site positioned himself. When and why an oesophagectomy may be indicated was explained very clearly by Jörg Zehetner in just two minutes.
The very next day, 18 August 2020, Jörg Zehetner could be heard again on Radio Bern1. This time on the topic of obesity, which is becoming more and more important as a disease in Switzerland and all other highly developed industrialised countries in the world. Here, too, Jörg Zehetner took a clear position on those affected and, with his many years of experience as a visceral surgeon, spoke about the classic methods of treating morbid obesity.
Here too, Jörg Zehetner impresses with his ability to present the essential treatment options in just two minutes.
Listen to the two podcast contributions from Radio Bern1 in full length here:
https://swiftcdn6.global.ssl.fastly.net/projects/5f3e31531d258/index.html?cb=abhioqr529cv93v8xj8x8
It should be noted that these short podcasts cannot replace a comprehensive and thorough diagnosis and counselling. If you think you are confronted with one of these two problems, contact one of the Swiss1Chirurgie clinics. A visit to the website www.swiss1chirurgie.ch can also be helpful. Extensive content on the subject areas is offered here. In addition, all contact details for Prof. Jörg Zehetner and the Swiss1Chirurgie clinics can be found there.
A threat to humanity
Morbid obesity is increasing rapidly worldwide
Go directly to the self-test: https://ch.run/20sekunden
Life always comes with particular challenges and some of them we like to think of as a threat to our own existence. Epidemics, pandemics, forces of nature, cancer, accidents, other serious illnesses and, last but not least, violence instil a good deal of fear and anxiety in each of us.
Yet there is a modern widespread disease that is much more dangerous and deadly in the long term than anything already listed here. We are talking about morbid overweight, which is also called obesity in different stages in professional circles. Far more people are affected by morbid obesity, including its accompanying symptoms and secondary diseases, than we generally realise. Trend: Rapidly increasing!
Oversupply of food and lack of exercise
Obesity is particularly rampant in the developed industrialised countries, for example in Europe, but also on the American continent. However, more and more regions in Asia are also affected, and obesity does not even stop at the African continent.
An overabundance of constantly available food, wrongly learned eating habits passed on to one’s own children, lack of exercise and a fast food culture that is often far too rich in fat and sugar are certainly partly responsible for obesity.
Know what is happening
But first and foremost, it is the people themselves who fall into the obesity trap due to lack of knowledge, lack of contextual thinking and out of convenience. And they often do so with their eyes open, but without a keen awareness of the consequences of poor nutrition. Liver disease, joint problems, circulatory problems, disorders in fat metabolism, shortness of breath, stroke and psychological impairments due to subsequent stigmatisation are only a sample of a wide range of concomitant and secondary diseases that can ultimately be traced back to morbid obesity. This is accompanied by a significant impairment of the quality of life and sometimes the only way to get a grip on the situation is to have surgery. And even that alone is not the solution to the actual problem, but only a last resort for people who are particularly severely affected by morbid obesity.
Obesity as a widespread disease threatens existence
From the medical view of the overall situation, it can indeed be concluded that in the longer term, humanity’s existence is threatened by the widespread disease of obesity. This may be an unimaginable scenario now, but it gains in threat potential when we consider the development of obesity on a global scale.
It is up to each individual to decide how to influence his or her diet and physical constitution. Provided there is a firm will to do so and the insight that the blessing of always having enough food in the existing abundance may not be a real blessing at all.
Determine your own score
We have presented a quiz at https://ch.run/20sekunden that everyone can use to determine their very own overweight risk score. Valuable conclusions for necessary action can be derived from the results. From the experience of decades of research and practical medical and surgical work with severely overweight people, we know that only timely action can offer a way out of morbid obesity. And often it is the early realisation that a change in lifestyle and eating habits can be the best step towards a healthier and ultimately happier life.
In view of the threat that morbid obesity actually poses, our recommendation is to use the simple quiz to determine one’s personal score with regard to possible medical conditions related to obesity. For many, this can be the first important step towards a more conscious approach to their own lives. And even if life itself always seems to be threatened by serious illnesses, accidents, worldwide pandemics or unavoidable forces of nature, we should never underestimate the dangers to which we voluntarily expose ourselves every day through too much and the wrong diet with a simultaneous lack of exercise.
With our quiz at https://ch.run/20sekunden you can quickly and easily determine your risk score and at the same time receive important information on what you can do now or should do urgently. Because there is nothing more precious than life.
Aftercare in the focus of obesity surgery
Interview with Dr Steffen, ZfbC
In an in-depth interview, Dr Steffen from the Centre for Bariatric Surgery ZfbC discusses the importance of follow-up care for overweight patients. In addition to the actual bariatric surgery, structured aftercare is of enormous importance. Only if those affected are actively involved in the process throughout their lives is sustainable success possible. A detailed article on the interview and the interview with Dr Steffen himself can be found here.
New information page for patients: www.nachsorge.ch
Aftercare in the focus of obesity surgery
Anyone who talks about bariatric surgery, such as stomach reduction or the formation of a tube stomach, must also talk about professional aftercare and further treatment for patients.
This is exactly what Dr Steffen from the ZfbC, Centre for Bariatric Surgery, does in the featured video interview. With over 30 years of experience and 3,600 stomach operations performed himself in the field of obesity surgery, Dr Steffen is one of the leading luminaries in this medical speciality in Switzerland.
Evaluation of the risks
Whether gastric banding, gastric bypass, stomach reduction or other techniques, there is always a certain risk of relapse for the treated patients. It is precisely the reduction of the recidivism rate, ZfbC, when it comes to professional aftercare following obesity surgery. Dr Steffen makes this unmistakably clear.
Obesity treatment is a lifelong process
It should also be clear that after an initial operation for the majority of those affected, there will be further interventions to ensure the success of obesity surgery. At the same time, this means that in the majority of cases, surgery alone will not be enough for the rest of one’s life. Accordingly, it is important to accompany and care for the patients continuously and individually in the aftercare.
Children in obesity surgery
According to Dr Steffen, children are not excluded from the problem of morbid obesity. Fat children usually also become fat adults, so that early intervention can make sense if there is an appropriate indication. It is important to note that the rules and regulations for bariatric surgery must also be observed for minors.
Follow-up care is the decisive success factor
Dr Steffen believes that ongoing follow-up care is more important than the timing of the surgical intervention. From experience, he knows that many patients do not take proper care of themselves after an initial overweight operation has been performed. However, it is also the professional colleagues who must be held accountable, as they do not always focus on special aftercare in their further care. Here, the ZfbC can definitely fill treatment gaps. One should understand morbid obesity similarly to an incurable disease, so that a good strategy for lifelong aftercare must be presented here as well. What Dr. Steffen cannot understand is the fact that he repeatedly encounters patients who are left alone in their problem situation after obesity surgery and are not sufficiently perceived.
Accordingly, the ZfbC would also like to open up to patients who have not been treated in a Swiss1Chirurgie clinic or an affiliated clinic. Here, anyone who complains about a wide range of problems after bariatric surgery should get a sympathetic ear and professional support. What definitely does not work is that patients are simply left to their own devices after obesity surgery with reference to their diet programme. This contradicts every ethical and medical claim.
It should also be clear in this context that anyone who cannot successfully deal with their excess weight before an operation will not be able to do so without help even after the operation has taken place.
Understanding aftercare as a standard
For Swiss1Chirurgie, structured aftercare is part of the standard in obesity surgery. Even though this is unfortunately not the case everywhere, the experts at Swiss1Chirurgie, together with the ZfbC, attach great importance to professional and structured aftercare in the best interests of the patient. This is the only way to ensure initial success, to identify problems in time and to build on the long-term success of the therapy. Anything else doesn’t make much sense.
It is also worth noting that deficiency symptoms can always occur due to the way the different treatment methods work. Such processes must of course be monitored and controlled to show patients how to compensate for certain deficiencies such as calcium deficiency or vitamin deficiency.
Follow-up care for overweight patients is a team effort at ZfbC. In addition to Dr Steffen himself, other specialist colleagues also devote themselves to the patients’ problems in special aftercare consultations. Around 8,000 patients are now being cared for. In the regulations, the Federal Office of Public Health requires follow-up over five years. However, the experts at Swiss1Chirurgie know that, in fact, lifelong follow-up of patients is sensible and necessary. Here, the legislative requirements obviously fall short.
Complications can occur at any time
The problems of the individual patients are very different. The aftercare must be correspondingly individualised. Some of the problems are real complications such as chronic abdominal pain, persistent diarrhoea, deficiency symptoms, vomiting or other functional problems. In principle, every affected person must expect that some kind of problems will occur over a short or longer period of time. Even if this ultimately does not affect everyone, it is still a clear proportion of patients who have to deal with certain problems after obesity surgery.
Alcohol and obesity
As Dr Steffen clearly explains, alcohol has a special effect on obesity and even more so on patients treated accordingly. In his opinion, alcohol has just as high a caloric value as pure fat, in addition to the typical symptoms of intoxication. Accordingly, it makes little sense or is even counterproductive for overweight patients to consume alcohol beyond a low level. The best thing would be to abstain completely from alcohol. This is also the aim of good aftercare.
With every intervention, the risk increases
Regarding the general risks in obesity surgery, Dr Steffen emphasises that laproscopic surgery as such is first of all extremely safe and associated with only a few risks. The first operation is always less risky than every subsequent one, although it also depends on how experienced the surgeons are in the respective clinics. Much more common are the complications that can occur after the procedures. First and foremost are deficiency symptoms, digestive problems and problems in the area of the oesophagus. This must always be expected after obesity surgery, which is why lifelong aftercare is also sensible and recommended. This must also be clear to the general practitioners and is already addressed in the first educational discussion.
Obesity and Corona
Currently, the corona virus plays a significant role in society as a whole. Those who are overweight must expect a more severe course after an infection due to their physical constitution. If overweight people already have breathing problems, these will certainly be even greater with COVID disease, even more so with assisted or artificial ventilation. It is difficult to decide not to operate on overweight people now, as they will then be much more affected in the event of an infection later on.
The role of general practitioners
The first way for overweight people who want to improve their situation is always to see their family doctor. The latter will then make a referral to the specialists in the given case. Here, the Swiss1Chirurgie clinics are recommended as competence centres for bariatric surgery. The family doctor could also be the first point of contact for appropriate information to the patient. In addition, we as Swiss1Chirurgie offer a comprehensive information service for all those affected. This ranges from our special consultation hours to the detailed and extensive information on the internet and via our app. However, information about any site or place on the internet is always associated with the risk of getting the wrong information. Here, Dr Steffen likes to refer to the pages of Swiss1Chirurgie, which, in contrast to any forums or chat rooms, provide extremely professionally correct, comprehensive and structured information.
Swiss1Chirurgie informs patients and endocrinologists
New set of rules for obesity surgery
From 01 January 2021, it will be possible to have obesity surgery from a BMI of 30+ with concomitant type 2 diabetes. One of the prerequisites is that diabetes can no longer be safely controlled by conventional means. Only a few specialist clinics are authorised to perform such operations. This also includes the clinics of Swiss1Chirurgie, which offer such procedures in the Helvetia Holding AG network. Learn more about the BAG’s decision.
Overweight surgery possible from BMI 30 with diabetes as of 2021
Being overweight is not something to be trifled with. All those affected know this just as well as we do as medical specialists. For years, the experts at Swiss1Chirurgie have been observing the development of obesity in modern industrialised countries. It is becoming increasingly clear that the proportion of overweight people is growing. Associated with this are not only the individual restrictions and complaints. Healthy societies quickly become sick societies through an oversupply of food at any time in any place and correspondingly wrong nutritional behaviour, whose lack is above all abundance.
So far, health insurers and medical organisations, together with politicians in Switzerland, have agreed that surgical interventions to reduce weight are only possible for a BMI of 35 or higher and are financed accordingly. It was completely ignored that a BMI of 35 or more is already an enormously high value, which is already associated with numerous secondary diseases and complaints. Such concomitant diseases not only complicate the lives of the patients themselves, but are often also a clear obstacle in the preparation and implementation of necessary obesity surgery.
From 2021 the threshold is BMI 30
In accordance with the interventions of the medical specialists and a close observation of the development, the politicians together with the medical profession have decided to lower the threshold value for bariatric surgery in the context of obesity surgery now to a BMI of 30, provided that the patients are affected by diabetes at the same time.
This long overdue decision will benefit patients who, despite being diagnosed with obesity and the corresponding symptoms, were previously not included in the group of patients for whom obesity surgery was an option.
This means that a wide range of conditions closely related to obesity can be treated much sooner and necessary and desired surgical interventions can also be carried out. This will have a lasting impact on the quality of life of people with a BMI over 30 and diabetes, and ultimately reduce the proportion of severely overweight people, along with the social and economic costs.
Advantages especially for humans
The decisive advantages of this decision now lie above all with those people who, with a BMI of 30 or more and diabetes, are already clearly affected by morbid obesity. Now the suffering of these people can be significantly shortened. This is also because it obviously does not make sense to wait for an enormously high BMI of 35 and more until a surgical intervention for weight reduction is made possible by the regulations.
A major advantage of this decision is that the extent of overweight and the associated concomitant and secondary diseases such as diabetes, cardiovascular diseases and arthrosis can be significantly reduced. The psychological suffering can also be significantly shortened and patients with a BMI of 30 or more with diabetes may now place themselves in the hands of the experienced specialists in obesity surgery. The Swiss1Chirurgie clinics are among the specialist medical clinics that will be authorised to perform surgical procedures to reduce excess weight from a BMI of 30 with diabetes from 01.01.2021.
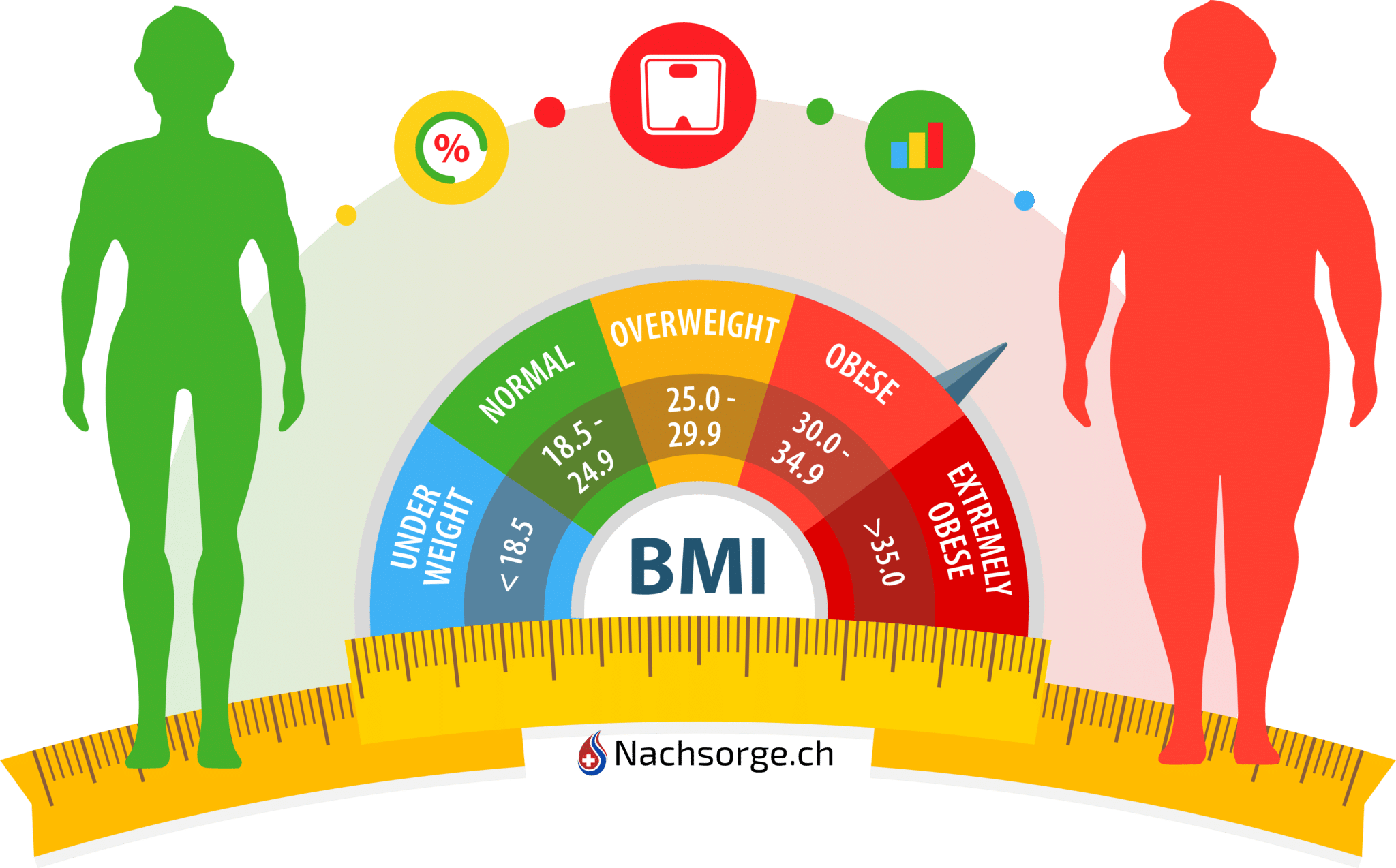
Determine your BMI here and find out whether and under what conditions you belong to the circle of possible candidates for obesity surgery.
In addition, we recommend that all severely overweight people contact a Swiss1Chirurgie clinic. By doing so, you will take the first step towards a better, healthier future in 2021 and use the possibilities of modern medicine to improve your life.
Contact Swiss1Chirurgie here.
Gastric balloon only a “crutch” for overweight patients
Those who suffer from morbid obesity look for quick solutions. The use of a gastric balloon promises such a quick solution. However, such a gastric balloon is nothing more than a “crutch” in the treatment of obesity. The obesity experts at Swiss1Chirurgie, the Centre for Bariatric Surgery ZfbC and the Gastroenterology Group Practice Bern know this. In the detailed article, the benefits of bariatric surgery are contrasted with the rapid effects of a gastric balloon. Here is the full report.
The gastric balloon – the best way to cheat yourself?
Why a gastric balloon is the worse alternative to bariatric surgery?
Those who suffer permanently from severe overweight and feel stigmatised by their social environment often look for quick solutions to reduce their body weight. People affected by obesity and the associated concomitant and secondary diseases want effective measures and treatments to change their life situation. The so-called gastric balloon promises such a quick remedy. Without any surgical intervention, without restrictive diets, in the wrong perception and even without a change in exercise behaviour, a quick weight reduction could be achieved with a gastric balloon. But the first impression is just as deceptive as the first successes.
How the gastric balloon works

The gastric balloon is usually inserted into the stomach by means of gastroscopy and filled with a saline solution in the same procedure. Recently, some centres have also been promoting a “swallowable” version – the balloon is swallowed and filled via a tube – without the need for a gastroscopy. This installs a foreign body in the stomach that significantly reduces the stomach volume available for food intake.
As a result, a feeling of satiety is produced even after eating comparatively small amounts of food, but this can be very deceptive. Because of this early onset of satiety, many patients think they can lose weight quickly, easily and permanently with the intragastric balloon without surgery. However, this is often accompanied by complaints such as nausea and frequent vomiting, which indirectly help to lose weight in a rather unpleasant way.
In fact, there are reports that the gastric balloon can be used to lose ten to 25 kilograms over a reasonable period of time. It should be remembered, however, that efficient weight loss attempts are less about quantity and more about the quality of the food. Anyone who consumes very high-calorie drinks, fatty foods or a lot of sugar-heavy food to satisfy their needs after the insertion of a gastric balloon will not automatically achieve success even with the reduced mass. Without a consistent change in diet and exercise, attempts to lose weight are hardly successful in the long term, even with the gastric balloon. Especially since a gastric balloon can only ever be used temporarily.
Self-deception with a system
Experts in the treatment of obesity speak of self-deception with a system when favouring a gastric balloon for weight reduction. After all, such a gastric balloon is a foreign body in the stomach and at best something like a crutch in the treatment of obesity. And a crutch is not a leg on which you can stand safely.
It is also worth considering that the gastric balloon is not a permanent solution. Depending on the quality, such a gastric balloon can remain in the stomach for a maximum of 3, 6 or, more recently, 12 months and must then be removed. Although a new intragastric balloon can be placed immediately, this only continues the actual self-deception.
From the reports of those affected, it can also be learned that in addition to some good successes, a large number of negative experiences can also be registered. This ranges from persistent nausea to spontaneous vomiting to an unpleasant feeling of fullness, which does not contribute to the patients’ well-being. If the intragastric balloon is worn for the recommended maximum period of six months, there is a risk that the balloon will lose the saline solution, which in itself is not tragic. Much more dangerous is that the then flaccid envelope of the balloon can migrate into the intestine and lead to a dangerous intestinal obstruction.
Bariatric surgery is the better methodology
Given the problems associated with the use of a gastric balloon, bariatric surgery is the better option in the vast majority of cases in patients with BMI over 30 kg/m2 with diabetes, or in patients with BMI over 35 kg/m2 without diabetes. The preferred methods are stomach reduction by forming a tube stomach or gastric bypass. Such interventions aim to consistently and permanently reduce the volume of the stomach or to virtually bypass the stomach. Both methods involve surgical procedures, but these are now performed as minimally invasive laporoscopic operations. In addition to the bariatric operations, further therapeutic offers are provided with the aim of achieving and securing long-term success in weight reduction. This means that in the vast majority of cases, surgical intervention is the better, more reliable and permanently more successful way to treat morbid obesity in the long term.
When the use of a gastric balloon can be useful
Even if a gastric balloon does not appear to be a target for long-term weight reduction, it can still be a sensible temporary solution in individual cases. For example, if a surgical intervention is not (yet) an option because of a very high excess weight. Then the gastric balloon can help to achieve a weight reduction that makes surgery possible. But that’s all.
If we consider once again that the intragastric balloon is basically a foreign body that can only be used temporarily and is ultimately only a “crutch” for weight loss, the intragastric balloon is ruled out as a long-term and efficient solution to the problem of obesity.
Counselling ensures best treatment results

Anyone who is confronted with the physical, social and psychological impairments caused by morbid obesity should seek specialist medical advice and professional care. A good place to start may be the Swiss1Chirurgie clinics, the Centre for Bariatric Surgery ZfbC or the Gastroenterology Group Practice in Bern. Here, patients are advised in detail, individually and openly about the chances, risks and possibilities of permanent weight reduction. Obesity experts are always concerned with long-term solutions and less with quick but less reliable success.
In a special consultation at Swiss1Chirurgie, patients also learn in which rather rare cases the temporary use of a gastric balloon in preparation for bariatric surgery can be useful. At the same time, however, it is always made clear that the use of a gastric balloon can never be the permanently helpful solution to a pathological obesity problem.
Adipositas-Podcast.ch – Know what’s what
With the obesity podcast, you can find the latest and essential information on obesity, its origins, development, consequences and treatment options at adipositas-podcast.ch. Here, real experts talk about the causes and development of morbid obesity, which, with its manifestations such as overweight, cardiovascular diseases, shortness of breath, organ diseases, diabetes, limited mobility and performance as well as social stigmatisation, severely restricts the lives of those affected. On adipositas-podcast.ch we always want to inform you professionally and comprehensively and at the same time show you ways to break the vicious circle of obesity.
One can accept obesity as a seemingly inevitable fate and surrender defencelessly to the dire consequences. But in the same way, obesity can also be understood in its development and ways can be found to return to a self-determined, happy and desirable life. What is your path?
Listen to experts from Swiss1Chirurgie, the Centre for Bariatric Surgery or the Gastroenterological Group Practice Bern and learn what obesity is, what it means for an individual’s life and which paths lead out of the disease. In this way, you will gain valuable knowledge that can significantly accompany your own path out of obesity. Testimonials from patients and sufferers and the knowledge of obesity experts will help you find your own way out of the fatal obesity career and lead a healthier and happier life.
Adipositas-Podcast.ch – Know what’s what
OESOPHAGECTOMY: THE TREATMENT OF OESOPHAGEAL CANCER
By DR. MED. JÖRG ZEHETNER, Professor (USC), Specialist in Surgery, esp. Visceral surgery
EVERY YEAR, AROUND 600 PEOPLE IN SWITZERLAND ARE DIAGNOSED WITH OESOPHAGEAL CANCER. MEN ARE PARTICULARLY AFFECTED, ACCOUNTING FOR THREE QUARTERS OF ALL CASES, AND ARE SIGNIFICANTLY MORE LIKELY TO FALL ILL THAN WOMEN. WE EXPLAIN TO YOU WHAT OESOPHAGECTOMY IS ALL ABOUT. REFLUX DISEASE IS THE BIGGEST RISK FACTOR FOR OESOPHAGEAL CANCER.
https://v.calameo.com/?bkcode=006115199b76ca4b1be03&mode=mini&showsharemenu=false&clickto=embed
A healthy liver promotes a healthy life

Fatty liver, non-alcoholic fatty liver, liver cirrhosis, liver cancer, hepatitis as infection of the liver and many other liver diseases are common. It is estimated that the proportion of people diagnosed with fatty liver in developed European countries is around 20 percent, with a certain number of unreported cases, as mild and symptom-free courses of the disease are hardly recognised.
A distinction is made between three degrees of severity of fatty liver, initially regardless of whether it is alcoholic or non-alcoholic.
- Mild fatty liver – In this case, less than one third of the liver cells are affected by excessive fatty degeneration.
- Moderate fatty liver – At this stage, a proportion of less than two-thirds but more than one-third of the liver is already excessively fatty.
- Severe fatty liver – In this degree of severity of fatty liver disease, more than two thirds of the liver cells are already excessively fatty.
Fatty liver cells result from the storage of fat in the liver cells, which ultimately significantly impairs the function of the liver as an important organ. Consequential diseases or concomitant diseases such as diabetes are not excluded, but are often a complication caused by the disturbed fat metabolism in the liver.
The severity of fatty liver disease can be determined by examining a tissue sample from the liver. In the process, a tiny part is taken from the organ and subjected to a fine-tissue examination. Examinations of the cholesterol level or the blood lipid values also provide valuable information.

Alcoholic or non-alcoholic fatty liver?
Many liver diseases are diagnosed in close association with the excessive consumption of alcohol. Anyone who is more familiar with the chemical composition of alcohol knows that it is a modified form of sugar, i.e. carbohydrates. An excess of carbohydrates is deposited in the body as fat and finds its place especially in the liver. Accordingly, many chronic alcoholics are affected by liver diseases up to severe forms.
But also, and this should be a cause for concern, a large proportion of non-alcohol-related liver diseases are spreading in society. Such manifestations of fatty liver are mainly due to wrong eating and living habits, which are mainly represented by excessively fatty and sugary diets. What the body cannot process, it not only deposits in the fat depots of the lower skin layers, but also in the liver, which then leads to fatty liver.
What to do for fatty liver?
Once an alcoholic fatty liver has been diagnosed, the only thing that helps is a strict
and consistent renunciation of alcohol. Only the radical renunciation of alcoholic beverages can still offer a spark of hope that the consequences of alcohol abuse on liver health can still be mitigated.
In the case of non-alcoholic fatty liver, the chances of recovery are relatively good, depending on the severity. What is important is a consistent change in diet combined with more active exercise. This change can be supported by so-called liver fasting, which we will look at in more detail in a separate section. In principle, it is always important to prevent scarring of the liver tissue, which is referred to in medical terminology as cirrhosis of the liver. Cirrhosis of the liver is beyond repair and represents a dangerous structural change in the liver tissue that cannot be reversed.
Once a fatty liver has been diagnosed, depending on its severity, it is important to make actual changes to halt and, if possible, reverse the process of fatty liver. Half-hearted measures help relatively little. Also because a relapse into old lifestyle and dietary habits will always lead to progressive damage to the liver.
Treatment of fatty liver with medication or surgery is not possible. In the case of a fatty liver, the only thing that can help is to tackle the causes, which are to be found either in excessive alcohol consumption, in the wrong diet that is too rich in fat, or in a combination of both. Some rare forms of fatty liver are due to medication or other episodes, but are negligible in this paper.
Who is affected?
If you follow the statistics, about 20 percent of our society is affected by non-alcoholic fatty liver. The age of patients ranges from 40 to 60 years, with women being affected by fatty liver slightly more often than men.
It is noteworthy that many patients with fatty liver are significantly overweight (obesity) or already suffer from diabetes in various stages. Elevated blood lipid levels are as common as the occurrence of metabolic syndrome.
Even if the actual causes of a fatty liver have not yet been fully researched, it can be assumed that there is basically a disproportion between energy intake and energy consumption. This means that in the long term or permanently, significantly more calories are supplied to the body than are actually consumed.
Even though fatty liver is often associated with alcohol abuse in the general perception, the proportion of non-alcoholic fatty liver is much higher than that of alcoholic fatty liver disease.
Liver fasting according to Dr. Worm – a good therapy for non-alcoholic fatty liver
A liver fast according to Dr. Worm is an effective means of individually and successfully combating fatty liver. Even without a specific medical diagnosis, but especially after a diagnosis of non-alcoholic fatty liver, liver fasting according to Dr. Worm offers excellent possibilities for a targeted and healthy defatting of the liver without overtaxing the organism. However, it must also be said that any form of dietary nutrition, including liver fasting according to Dr. Worm, does not work without renunciation and one’s own will.
This is how liver fasting according to Dr. Worm works
Dr. Nicolai Worm is one of the best-known nutritionists of our time. Based on years of experience in nutritional counselling and supported by current scientific findings, Dr. Worm has developed liver fasting with Hepafast together with the nutritional physician Dr. Hardy Walle, MD. Such a diet is by no means new territory, but is based on the experience of many decades of research, science and practice.
The special thing about the Hepafast cure is that it specifically addresses the requirements and physical circumstances related to a fatty liver. This means that with the targeted Hepafast liver fasting cure, which is limited to a few weeks, the fat levels of the liver can be specifically influenced.
If the liver fasting cure according to Dr. Worm is carried out correctly, the fat metabolism is naturally influenced, which in the majority of cases also leads to a general weight loss. Both the blood fat values and the liver fat values recover noticeably, the success of liver fasting can be observed and experienced by the person doing it. Unlike many other diets, the feared yo-yo effect is not to be expected, as the Dr. Worm liver fast is not a starvation diet, but is accompanied by valuable ingredients in an easy-to-prepare drink.
Of course, liver fasting with Hepafast makes no sense if the diet and lifestyle in general are not changed at the same time. However, as Hepafast works naturally and is filling, continued excessive food intake is neither felt nor factually necessary. The affected persons therefore eat more sensibly and healthily, do not have to starve themselves and simply supplement their diet with Hepafast. This leads to a significant decrease in fat levels and thus to improved health, which is also noticeable in performance after just a few weeks.
When is liver fasting according to Dr. Worm useful?
In principle, liver fasting according to Dr. Worm always makes sense at the latest when symptoms of a fatty liver are noticed. However, a fatty liver in the first degree of severity is not associated with any individual complaints and is therefore usually not even noticed.
It is good that liver fasting according to Dr. Worm can also be carried out preventively, without deficiency symptoms or too abrupt changes in lifestyle. Step by step, users can familiarise themselves with the mode of action of liver fasting and are then guided themselves to make their lifestyle and eating habits more sensible.
Liver fasting according to Dr. Worm is particularly recommended after the cold season. In winter, most people exercise a little less anyway, rich and fatty food is often part of everyday life in winter, and around Christmas and spring is the best time to activate the body again. Especially since Lent is in full swing then anyway. In addition, liver fasting according to Dr. Worm with Hepafast can be used practically any time of the year.
This is how liver fasting with Hepafast works
In many years of nutritional research, Dr. Nicolai Worm and Dr. Hardy Walle, MD, have put together a formula that has a measurably positive effect on liver fat values. The special composition and easy handling of the Hepafast liver cure helps to boost fat burning and successfully reduce the storage of fat in the liver cells. Finally, the ingredients of the Hepafast cure also have an effect on the fats already stored in the liver and can effectively break them down.
A prerequisite for a successful liver fasting cure with Hepafast remains a sensible change in lifestyle and dietary habits. Hepafast is not a miracle cure, but a nutritionally compounded support for defatting the liver and for overall better eating habits. Accordingly, Hepafast is not a food supplement, but replaces part of the diet with liver-active components when used as intended.
In concrete terms, this may mean that lunch or another meal is replaced by a Hepafast Shake prepared as intended. There is no need to fear a feeling of hunger, as Hepafast is satiating and at the same time can break down fat molecules in the body. The fear of an unbalanced diet or malnutrition is also not justified, as other meals can also be taken when using Hepafast, which then contain the substances required by the body. A Bodymed Hepafast liver cure is not a diet that focuses primarily on renunciation, but rather a targeted influence on fat burning in the body. Ideally, Hepafast not only helps burn fat cells, but can also promote weight loss. In addition, the effects of liver fasting with Hepafast boost the body’s own forces and energies, which can generally lead to an improved sense of well-being and higher performance. It is important to know that in liver fasting according to Dr. Worm, the focus is not on radical or large-scale weight loss, but on naturally flawless liver function.
Experience reports with Bodymed Hepafast Liver Fasting according to Dr. Worm
Years after the first introduction of liver fasting according to Dr. Worm, there are thousands of enthusiastic and successful users who have not only been able to reduce the degree of liver fatty degeneration, but also to take preventive action against possible liver fatty degeneration. And that with relatively little effort and sacrifice, but a liver-healthy dietary pattern that is excellently supported by Hepafast.
In the Swiss1Chirurgie clinics, we also support and recommend liver fasting out of the knowledge that overweight people in particular often suffer from non-alcoholic fatty liver, even if they do not always feel it immediately. Healthy liver function plays a significant role in well-being. Conversely, a balanced, varied and healthy diet always promotes liver health. This can be supported very well with Hepafast liver fasting according to Dr. Worm.
Here are some feedbacks from people who regularly do the liver fasting according to Dr. Worm.

“As a player and as a coach, I have been paying a lot of attention to my diet for years.
I tried out many different ideas and projects to be able to talk to my players about performance optimisation.
3 years ago I consciously detoxified my liver for the first time on recommendation.
I was curious to see what the body would do to me.
14 days of iron discipline. Protein shake, vegetables, counting calories was the routine that accompanied me every day.
The result: 5 kilos lost, vital, motivated, dreams, fit in spirit, conscious handling of nutrition and real enjoyment.
Not once did I feel hungry. I was allowed to get to know many interesting, creative menus.
In short, “it was worth it.”
I can highly recommend liver fasting with a clear conscience.
Bottom line: do something good for yourself while you wait for happiness.”
Martin Andermatt, football player and coaching legend

“Thanks to liver fasting, I experienced unique things at the beginning of each of the last years.
Whether on a snowshoe tour through the Ottmar Hitzfeld GsponArena or in the home office, whether at the CSI event in Basel or the Lauberhorn Races in Wengen, 14 days changed
my consciousness with liver fasting. For 14 days, the perfect-tasting Bodymed shake was my faithful companion and made every single day a pleasure.
I was able to experience positive things: Better well-being, deeper sleep, reduced fatigue, healthy eating, weight loss. And liver fasting brings even more
welcoming side effect – it saves valuable time, is easy on the wallet and helps you learn new cooking habits.
“Liver fasting means 5 star health for me.”
And who knows, with a little luck, the intense dreams will come true thanks to liver fasting … “
Fabian Furrer
“I treat myself to a liver fasting course of Hepafast once or twice a year. With a BMI of 24, I do this not to regulate my weight, but because it means wellness for my body. I feel much fresher after the cure, which is also confirmed by my blood values (cholesterol and liver values).
The most important thing for me, however, is that I don’t have to go hungry at any time with the Hepafast cure! The shakes taste good and give a good feeling of satiety. The recommended meals are easy to prepare and bring a lot of variety into the diet. And last but not least: I’m on the road a lot, but I can easily take the shakes and vegetable snacks with me and prepare and enjoy them “on the go”.”
Markus Fuhrer

“I am very satisfied with the liver fasting according to Dr. Worm, Hepafast, which was prescribed to me by Dr. Jörg Zehetner, MD. My laboratory values, especially cholesterol, are now all at a good level and I have lost 15 kg in one year because my eating habits have changed after the fast. I will repeat the cure every spring to stay in shape.”
Erika Fuhrer
Now, the series of experiences with Hepafast and a liver fast according to Dr. Worm could be extended almost indefinitely. However, we are of the opinion that only one’s own trial and error with one’s own personal experiences in liver fasting is really useful and meaningful.
Accordingly, we at Swiss1Chirurgie recommend that you make your own experiences with liver fasting according to Dr. Worm. “Because there is nothing good unless you do it!”
You will receive appropriate professional and medical advice on liver fasting according to Dr. Worm with Hepafast gladly and in detail in every Swiss1Chirurgie clinic and also in the other affiliated clinics within Helvetia Holding AG.
Expert advice on liver fasting: